Blog, Physiotherapy
Rewiring Pain: How Dry Needling Helps Reset the Body
If you’ve been living with stubborn pain that just won’t go away, chances are you’ve explored various treatments; some helpful, others less so.
One technique gaining traction in modern physiotherapy is dry needling. It’s used to address muscular pain and dysfunction, and it does so by working with the body’s own systems to bring relief and restore movement.
I’m Mattias McAndrew, a physiotherapist with over eight years of experience in musculoskeletal rehabilitation.
In clinical practice, dry needling has proven to be a valuable tool – not just for relieving symptoms, but for helping the nervous system “rewire” its response to pain (Shah, Gilliams, & Danoff, 2015).
What Is Dry Needling?
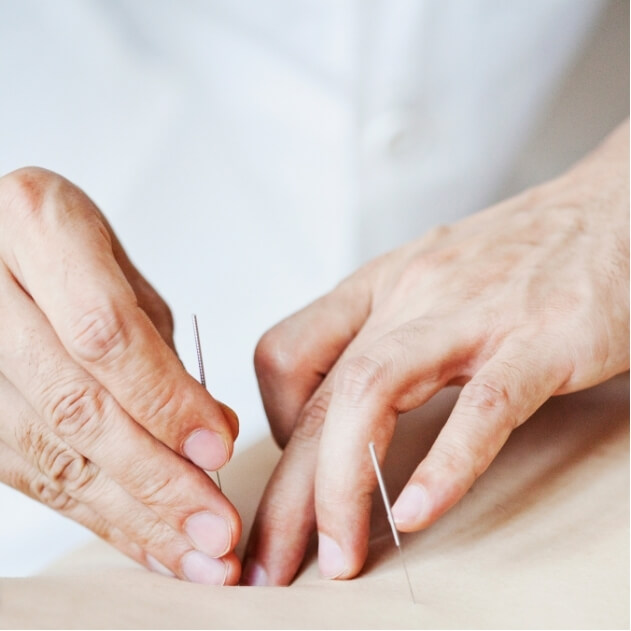
Dry needling involves the insertion of a fine, sterile needle into specific points within tight bands of muscle known as myofascial trigger points.
These spots often develop in response to overuse, injury, or ongoing tension.
Although dry needling and acupuncture both use thin needles, their principles differ significantly.
Acupuncture follows traditional Chinese medicine, while dry needling is based on contemporary anatomical and physiological understanding (Dommerholt & Fernández-de-Las-Peñas, 2018).
How Does It Work?
- Modulates Overactive Muscles
Trigger points are known to display abnormal electrical activity and excessive tension. Inserting a needle can disrupt this activity, often producing a local twitch response; a quick, involuntary contraction. This is thought to reduce muscle tone and desensitise spinal cord pathways involved in pain processing (Shah et al., 2015).
- Activates the Body’s Natural Pain Relief System
Needling stimulates sensory nerve fibres, which in turn activate the release of endogenous opioids; our body’s natural painkillers, such as endorphins and enkephalins. These substances engage descending pain-inhibitory pathways, helping to reduce the sensation of pain (Kietrys, Palombaro, & Azzaretto, 2013).
- Improves Circulation and Tissue Health
The mechanical stimulation from the needle enhances blood flow to the affected area, facilitating the removal of inflammatory chemicals and supporting tissue repair through better oxygen and nutrient delivery (Dommerholt & Fernández-de-Las-Peñas, 2018).
- Restores Chemical Balance in Muscles
Research has shown that trigger points contain elevated levels of pain-related substances like substance P and CGRP. Dry needling can help normalise these chemical imbalances, reducing local sensitivity and contributing to muscle recovery (Shah et al., 2015).
Clinical Uses
Dry needling is often integrated into treatment programs for:
- Mechanical neck pain and cervicogenic headaches
- Chronic low back pain and lumbopelvic dysfunction
- Shoulder injuries, including rotator cuff tendinopathy
- Post-surgical muscular pain
- Generalised myofascial pain syndromes
It’s most effective when combined with a comprehensive approach that includes exercise rehabilitation, manual therapy, and tailored education (Fernández-Carnero et al., 2017; Cotchett et al., 2014).
Safety and Training
Dry needling is considered a safe and low-risk technique when performed by trained clinicians.
Minor side effects such as temporary soreness or bruising can occur, but serious complications are rare.
Proper anatomical knowledge and skill are crucial for effective and safe application (Dommerholt & Fernández-de-Las-Peñas, 2018).
Final Thoughts
Dry needling is more than a short-term fix. It can facilitate meaningful changes in how the body responds to pain and supports tissue recovery.
When integrated into a broader rehabilitation program that includes exercise, manual therapy, and patient education, it has been shown to improve clinical outcomes in various musculoskeletal conditions (Cotchett et al., 2014).
While it’s not a cure-all, dry needling offers a valuable tool in the physiotherapy toolkit particularly for individuals dealing with persistent or complex pain.
Everyone’s situation is different. If you’re wondering whether dry needling could complement your recovery, feel free to give us a call on 1800 992 999 or book a consultation with one of our experienced physiotherapists.
 |
Written By:
Mattias McAndrew (Head Physiotherapist) Bachelor of Physiotherapy (Hons) |
References
Cotchett, M. P., Landorf, K. B., Munteanu, S. E., & Raspovic, A. M. (2014). Effectiveness of trigger point dry needling for plantar heel pain: A randomized controlled trial. Physical Therapy, 94(8), 1083–1094. https://doi.org/10.2522/ptj.20130255
Dommerholt, J., & Fernández-de-Las-Peñas, C. (2018). Trigger points and myofascial pain: Pathophysiology and evidence-informed diagnosis and management. Jones & Bartlett Learning.
Fernández-Carnero, J., Cleland, J. A., Palomeque-del-Cerro, L., Sánchez-Infante, J., & Arias-Buría, J. L. (2017). Effectiveness of dry needling for myofascial trigger points associated with neck pain: A randomized controlled trial. Journal of Orthopaedic & Sports Physical Therapy, 47(1), 11–20. https://doi.org/10.2519/jospt.2017.7096
Kietrys, D. M., Palombaro, K. M., & Azzaretto, E. (2013). Effectiveness of dry needling for myofascial trigger points associated with neck and shoulder pain: A systematic review. Journal of Orthopaedic & Sports Physical Therapy, 43(9), 620–634. https://doi.org/10.2519/jospt.2013.4668
Shah, J. P., Gilliams, E. A., & Danoff, J. V. (2015). Biochemical milieu of myofascial trigger points compared to unaffected skeletal muscle. Physical Medicine and Rehabilitation Clinics of North America, 26(2), 247–258. https://doi.org/10.1016/j.pmr.2014.10.004


