What is Plantar Fasciitis?
The plantar fascia is a thick band of connective tissue that stretches from the heel bone to the toes. The plantar fascia plays an essential role in providing the foot with energy storage and propulsion through elasticity while walking or running, as well as passive arch support at all times.
Plantar fasciitis, sometimes referred to as plantar heel pain, is the term that describes the plantar fascia becoming inflamed or painful. This is the single most common cause of heel pain. Plantar fasciitis can also result in mid foot pain on the sole of the foot. Plantar fasciitis is typically felt early in the morning and after periods of rest.
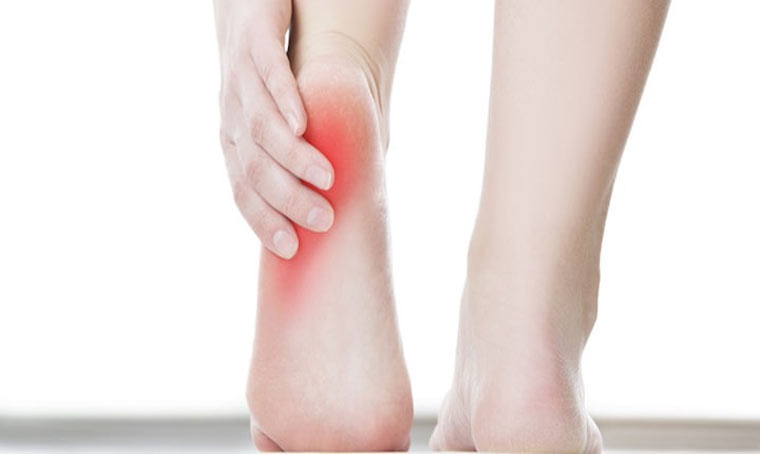

Common Symptoms of Plantar Fasciitis
Plantar fasciitis typically causes sharp, stabbing pain at the bottom of the heel or along the arch of the foot.
Common symptoms include:
- Pain is at its worst with the first steps in the morning or after long periods of rest.
- Pain during or after long periods of standing or walking.
- Tenderness along the medial heel or mid-foot area.
- Tightness or discomfort when flexing the toes upward.
- Swelling or mild inflammation near the heel.
If left untreated, plantar fasciitis can worsen over time and significantly impact physical activity and daily movement.
You may hear the term plantar fasciopathy, which describes longer-term changes in the plantar fascia when the condition becomes more chronic. While plantar fasciitis involves early inflammation, plantar fasciopathy refers to tissue degeneration that can develop over time if the problem persists.
What caused my Plantar Fasciitis?
The cause of plantar fasciitis pain is often difficult to pinpoint, as it rarely begins suddenly. Most often, those developing plantar fasciitis partake in impact or running activities, particularly if those activities involve sprinting and/or jumping (and landing on the feet).
It is also commonly diagnosed in those with flat feet or over-pronators. This can often lead to pain with prolonged standing, or any activities involving walking, running or jumping.
Occasionally, direct trauma can result in a plantar fascia rupture causing sharp pain and inflammation in the arch and heel. Structural changes in the heel, such as the development of heel spurs, can contribute to the development of plantar heel pain, however not everyone with heel spurs will develop plantar fasciitis.
Preventing Plantar Fasciitis
To help prevent plantar fasciitis from occurring or recurring:
- Wear supportive shoes with good arch support and cushioning.
- Avoid walking barefoot on hard surfaces for long periods.
- Maintain calf flexibility through regular stretching.
- Gradually increase physical activity levels to avoid overloading the plantar fascia.
- Use orthotics if you have flat feet or abnormal foot mechanics.
- Strengthen the foot and ankle muscles to improve stability and reduce strain on the plantar fascia.
Our physiotherapist will guide you on specific strategies suited to your biomechanics and lifestyle.

How can you help me with my Plantar Fasciitis?
Your physiotherapist will take a thorough history of your plantar fascia pain, as well as your activity history in order to best diagnose your injury. They will also perform a full physical examination of your hip, knee, ankle and foot in order to provide you with the best possible treatment plan.
Typically, your treatment will involve manual therapy and taping techniques in order to help improve your movement and reduce your pain. They will also give you stretching exercises, including Achilles tendon stretching, as well as strengthening exercises for your foot and calf muscles designed to improve your function and significantly reduce pain.
You can also expect your physiotherapist to address your walking and running biomechanics, and make suggestions regarding orthotics or shoe choices, in order to prevent any future recurrences or development of chronic plantar fasciitis.
What should I do to avoid aggravating my Plantar Fascia?
- AVOID activities that aggravate your pain until you have seen your physiotherapist
- REMAIN ACTIVE, while avoiding aggravating activities.
- For RELIEF, applying ice to the area may help to reduce some pain and inflammation. Wrap the ice to avoid direct contact with your skin
- For RELIEF, gentle massage of the soles of the feet can provide some relief.
- RECEIVE physiotherapy care to get your joints, ligaments and muscles performing to their optimum level.
Keep good care of your body and your physiotherapist will continue to monitor your condition. Once your Plantar Fasciitis has resolved you will be able to resume your full activities without worrying about future flare-ups.
Sports Physio for Plantar Fasciitis
Athletes and active individuals place unique demands on their bodies — and plantar fasciitis can be particularly disruptive to your training and performance.
At M Physio, our sports physical therapy approach goes beyond pain relief to address the root causes of injury and help you safely return to sport at your best.
When treating athletes with plantar fasciitis, we focus on:
- Biomechanical Analysis: Identifying imbalances like feet flat along the soles (fallen arches) or altered running gait that place excessive strain on the medial heel and plantar fascia.
- Targeted Strengthening: Progressive loading programs to strengthen the calf muscles, foot stabilisers and metatarsal bones for better shock absorption and propulsion.
- Calf Stretching and Mobility Work: Specific exercises to improve flexibility of the Achilles tendon and plantar fascia are crucial for reducing tension on the affected leg.
- Pain Management and Load Modification: Strategies to maintain physical activity while protecting the injured tissue, including taping, manual therapy and advice on wearing supportive shoes.
- Return-to-Sport Planning: Gradual reintroduction of running, jumping and sport-specific drills to ensure safe and confident performance.
Our goal is not just to treat the symptoms — but to build a stronger, more resilient foundation so you can stay active long-term. Patient education is a key part of every program, helping you understand injury prevention and how to manage any flare-ups. Find out more about our sports physio services.
If plantar fasciitis is interfering with your sport, book a consultation today and start your recovery the right way.
Common Exercises recommended for Plantar Fasciitis
Specific stretching and strengthening exercises are an important part of plantar fasciitis recovery. Your M Physio physiotherapist may recommend:
Calf Stretching: Helps relieve tension in the affected leg and Achilles tendon.
Plantar Fascia Stretch: Helps reduce stiffness and improve flexibility in the arch of the foot.
Towel Scrunches: Builds strength in the small muscles of the foot and metatarsal bones.
Patient education is critical to ensure these exercises are done safely and progressively for long-term pain management and injury prevention. We recommend you follow your plantar fasciitis physio’s personalised advice.
Plantar Fasciitis Physio FAQs
How can I alleviate pain from plantar fasciitis?
Alleviating pain often starts with reducing inflammation and supporting the plantar fascia. Applying ice, resting the affected leg, performing gentle calf stretching and wearing supportive shoes are key strategies. Your physiotherapist will also provide manual therapy and targeted exercises as part of your personal pain management plan.
Should I stop exercising with plantar fasciitis?
Not completely. Staying active is important, but you should modify or avoid activities that cause sharp pain. Low-impact exercises like swimming or cycling can help maintain fitness without overstressing the plantar fascia.
How long does plantar fasciitis take to heal?
Recovery time varies, but with proper physiotherapy, most patients with plantar fasciitis improve significantly within 6 to 12 weeks. Chronic cases may take longer if not managed early.
What shoes should I wear for plantar fasciitis?
Look for shoes with firm arch support, cushioned soles and a slight heel lift. Avoid completely flat shoes or worn-out sneakers. Wearing supportive shoes at all times — even indoors — is critical for pain relief and healing.
Can plantar fasciitis come back after treatment?
Yes, plantar fasciitis can recur, especially if the underlying causes (like poor footwear, flat feet or tight calves) are not addressed. Following your physiotherapist’s prevention and maintenance advice reduces the risk of recurrence.
When should I see a doctor for plantar fasciitis?
You should see a healthcare professional if your heel pain persists for more than a few weeks despite rest and self-care, if the pain worsens, or if you have difficulty walking. Early physiotherapy intervention can help avoid more invasive treatments like bone joint surgery.
What is the role of a night splint in the treatment of plantar fasciitis?
A night splint holds the foot in a gently stretched position overnight, helping to maintain flexibility in the calf muscles and plantar fascia. For many patients with plantar fasciitis, using a night splint can significantly reduce morning stiffness and pain.
Why does plantar fasciitis often affect the medial heel?
The medial heel bears much of the load during walking and running. If you have biomechanical factors like flat feet (fallen arches) or overpronation, this area can become stressed, leading to microtears in the plantar fascia. Targeted strengthening and supportive footwear can help protect this vulnerable area.
Could plantar fasciitis ever require bone joint surgery?
Bone joint surgery is rarely necessary. Most patients recover fully with conservative treatment, including physiotherapy, calf stretching, orthotic support and patient education. Options such as shockwave therapy, low-level laser therapy or surgery are considered only when non-invasive pain management has been unsuccessful over several months.
How does physical activity fit into my recovery?
While it’s important to avoid high-impact activities that aggravate your symptoms, maintaining safe levels of physical activity is crucial. Your physiotherapist will guide you on modifying activities to support healing without overloading the plantar fascia or metatarsal bones.
What advice do you give for wearing supportive shoes?
Wearing supportive shoes with firm arch support and cushioning under the heel is essential for patients with plantar fasciitis. Avoid flat or unsupportive footwear, which can strain the plantar fascia further. Your physiotherapist may also recommend orthotics for added protection.